PM-JAY: To enable PMJAY to debut ‘quickly and seamlessly,’ information technology had to be coordinated in such a way that the ‘time-to-launch’ was kept to a minimum. IT has been a strong backbone for the scheme’s implementation across the country from its inception. The essential technological components are listed below.
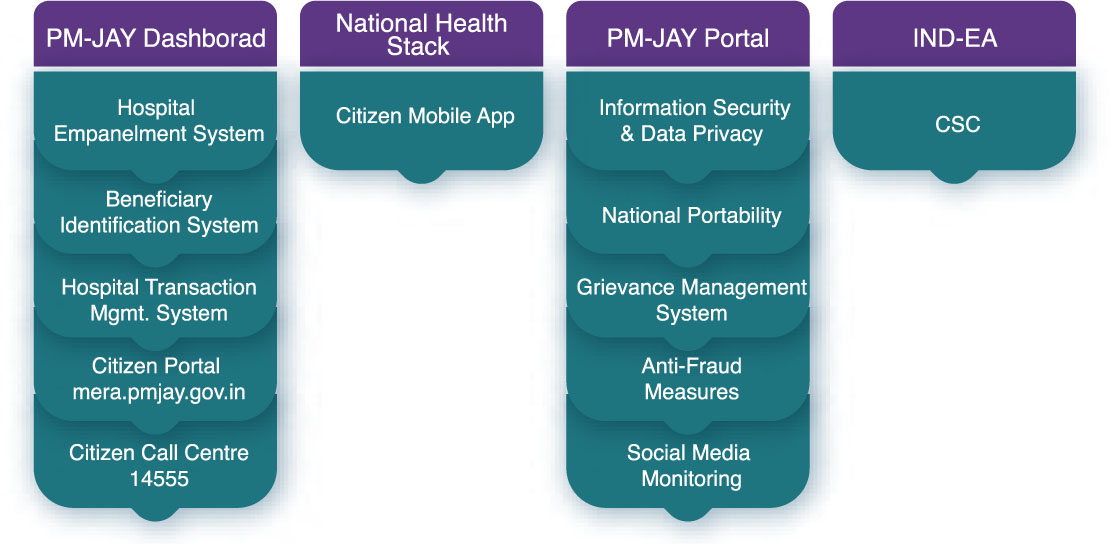
Key Technology Blocks of PM-JAY
PMJAY Dashboard: This allows you an aggregated and drill-down view of the PMJAY Data Warehouse’s numerous datasets. Is used for real-time transaction reporting, performance evaluation, and identifying usage trends.
Hospital Empanelment System: This allows hospitals to be registered and approved for empanelment. In addition, this system will include features for hospital quality assurance.
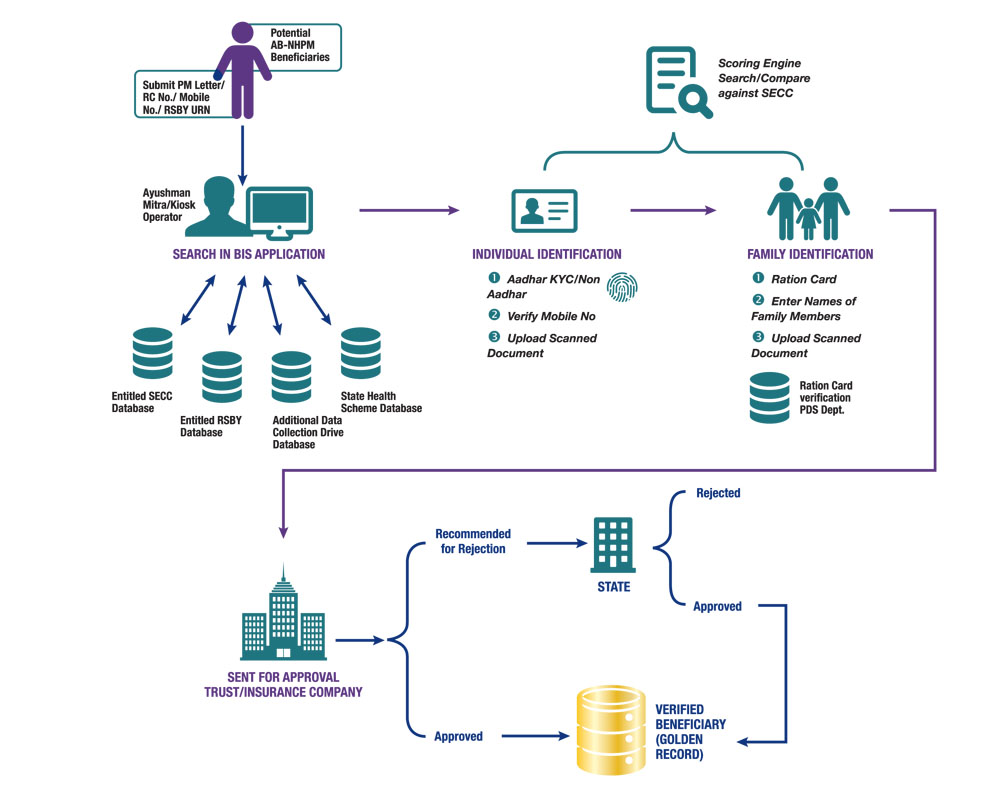
Beneficiary Identification System (BIS): This enables beneficiaries to be found using SECC or APIs, and it supports both Aadhaar eKYC (electronic Know Your Customer) and non-Aadhaar-based KYC for authentication.
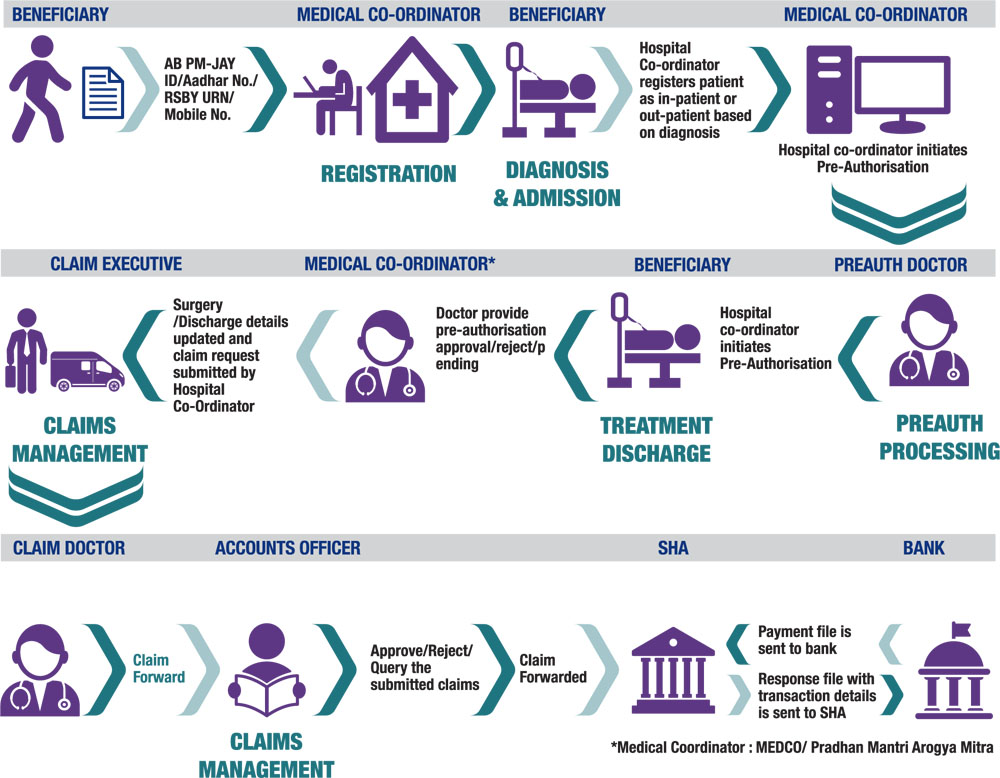
Transaction Management System (TMS): This enables the collection of in-patient data during admission, treatment, and discharge, as well as the submission of hospital claims and financial settlements. It uses an Application Program Interface to connect to other state-based and external systems (APIs).
Citizen Portal (mera.pmjay.gov.in): Citizens can examine the beneficiary database to see if they are eligible for the program. Because the popular self-help tool is mobile responsive, it allows for large-scale searches right at the field level.
Citizen Call Centre (14555): A national toll-free number backed by 400+ multilingual, multi-location call center services allows beneficiaries to learn about their eligibility, identify the nearest hospital, Common Service Center, and more. The phone center’s service offerings have been expanded to include beneficiary feedback and grievance resolution.
National Health Stack: Following a design philosophy, the NHS will allow PM-JAY to collect data that may be used to improve scheme design and allow for more inclusion/universalization in the future. The National Health Claims Platform (NHCP) is being developed, as is the upgrading of existing PM-JAY systems. These frameworks will pave the path for market-driven service delivery products to be developed for the regulated insurance program.
PM-JAY Portal: The platform is being upgraded to accommodate back-office tasks as well as being a single source of all information and content relevant to the program. The portal serves as a front end to the Grievance Management System, allowing users to discuss best practices, Standard Operating Procedures (SOPs), Policies, and Guidelines.
India Enterprise Architecture (IND-EA): Followed as a principle to enable the development of future-ready enterprise architecture for PM-JAY and NHA.
Information Security & Data Privacy Policies: Consider the many check-lists imposed on the IT Ecosystem – Service Providers and Consumers – to assure end-to-end data security and privacy for beneficiaries. To ensure compliance, evaluations are conducted on a regular basis.
National Portability: The IT system, which is unique to the scheme, has enabled the beneficiary to take their benefits with them wherever they go. Only by building solutions that allow for real-time integration and data interchange throughout the IT environment has this been achieved.
Grievance Management System: Beneficiaries and whistle-blowers can now record grievances, which the NHA/SHAs can then ‘take-to-closure.’ The technique ensures the griever’s anonymity as a critical component in creating confidence among beneficiaries.
Anti-Fraud Measures: A ‘Man-Machine’ approach has been proposed as part of the IT landscape to combat fraudulent transactions and entities. The model will produce triggers for questionable transactions and entities, as well as allow investigations into such transactions to be closed. To support investigations at the state level, a National Anti-Fraud Unit and a State Anti-Fraud Unit have been established.
Citizen Mobile App: Allows enrolled beneficiaries to check their current ‘wallet balance’ in the plan, search for the nearest hospitals, and submit comments on the hospitals’ services. As a simple personal tool, the recipients will be able to track their use of the benefits they are entitled to.
Common Service Centre (CSC): CSCs, as a service delivery partner, expand the scheme’s reach in rural India through their Gram Panchayat network. Through its network, CSCs have assisted in not only communicating about the plan but also in assisting potential beneficiaries in determining their eligibility and authenticating eligible beneficiaries.
Awareness and Communication
The most important part of PM-JAY is getting beneficiaries aware of the scheme because it is an entitlement-based scheme with no advance enrolling process. To educate beneficiaries about the scheme, information, education, and communication initiatives must be carried out. Leaflets, pamphlets, hoardings, TV, radio spots, and other forms of communication are vital components of a comprehensive communication plan for spreading desired messages to the target audience.
NHA has designed a detailed communication strategy that will be applied at both the national and state levels. NHA is also working with states to improve overall cooperation and ability in order to implement and create the communication plan needed to raise awareness at the state level.
Because of the high number of persons affected by PM-JAY, there is a pressing need to raise awareness with the correct message, through the right media, and in the right period. Following the Cabinet’s approval of the scheme on March 21, 2019, IEC activities began immediately. The first major initiative, the Additional Data Collection Drive (ADCD), was carried out by participating in the Ministry of Rural Development’s “Gram Swaraj Abhiyaan” on 30 April 2018, dubbed “Ayushman Bharat Diwas,” to inform people about the upcoming scheme benefits and entitlement checks by involving ASHA, ANMs, and Gram Sevak in over 3 lakh villages across the country.
For increasing awareness, various posters, banners, and other materials were developed and distributed in Hindi and regional languages across all camps and village gatherings. All beneficiary families received a letter from the Hon’ble Prime Minister informing them of their scheme entitlements and providing them with a family card with a unique family ID. NHA has created standardized design materials that are being utilized by states to inform beneficiaries about the program. To reach beneficiaries and other stakeholders, many communication channels such as print media, television, radio, social media, and so on are used. For this objective, a communication strategy, as well as an IEC guidebook, have been established.
A dedicated online page for the project has been built at www.pmjay.gov.in to give all information about the scheme to all stakeholders. Here you will find all important information and connections, such as a list of impaneled hospitals, an Am I Eligible page, a grievance redressal portal, a gallery, and operational instructions.
Support Systems
Apart from the critical components of the PM-JAY ecosystem mentioned above, there are a few other key components that work as a support system for the scheme’s smooth implementation.
Capacity Development
Capacity-building efforts under PM-JAY aim to include all areas of creating and growing sustainable and robust institutions and human resources, rather than only training. There are three parts to capacity building in PM-JAY:
- Setting up sustainable institutional structures,
- Building and strengthening the human resource and institutional capacity, and
- Maintaining knowledge and expertise through the use of proper tools and knowledge management. The institution’s, as well as each of its personnel’s, roles were defined at the national, state, and district levels, as were the precise skill sets required. This group of people was further divided into roles, with relevant knowledge and skill areas drawn out for capacity building.
The NHA has taken the lead in identifying needs, making funding available, developing strategies to enable states to engage in capacity-building initiatives, and providing technical assistance to states. The NHA is developing standardized learning content on designated theme areas. As part of their annual training strategy, states can personalize these materials and distribute them using multiple approaches.
To ensure efficacy and efficiency, monitoring and quality assurance measures with feedback mechanisms have been implemented. To support the capacity-building initiatives in PM-JAY, partnerships and networks are being formed with government and non-government entities with experience in several disciplines.
Capacity-building measures in PM-JAY began with SHA officials receiving training, followed by workshops for people from several portfolios such as IT, fraud control, and claim handling. There were also workshops for ISAs and banking partners. Before the start of the program, master trainers were formed at the state level, who then trained over 10,000 Pradhan Mantri Arogya Mitras (PMAMs) at impaneled hospitals. To support State and district-level training, learning materials were also made available through the portal.
With the help of the National Skill Development Council (NSDC), an e-learning platform for training and certifying Arogya Mitras is currently being built. In the next few days, there will be a variety of workshops, cross-learning forums, and thematic training.
Monitoring and Evaluation
Monitoring and Evaluation (M&E) are critical for effective implementation and ensuring the intended results of such a large insurance scheme PM-JAY Monitoring and Evaluation (M&E) are critical for successful implementation and ensuring the intended results of a large insurance scheme. Through the following functional domains, the NHA at the central level keeps track of these UHC characteristics (coverage, benefits, and financial protection) on a regular basis:
- Beneficiary management
- Transaction management
- Provider management
- Support function management (comprising functions such as capacity development, grievances, frauds, abuse, call center, etc.)
At the national level, a powerful real-time online MIS is in place to review Key Performance Indicators (KPIs) and the achievement of results related to the domains’ aims. The numerous dashboards created with business intelligence technologies assist in spotting gaps and providing an overview of the results achieved.
To name a few, the operations dashboard provides an update of beneficiary information system KPIs, the pre-auth dashboard facilitates access to state and district-level pre-auth distribution, as well as the status of impaneled hospitals, and the portability dashboard provides an overview of interstate and intrastate claim portability, as well as KPIs on claim portability by specialty, procedure, age, and gender.
The NHA software is used by the majority of states that do not have their own schemes. States with their own systems, on the other hand, use either the above or their own software with API integration to assure data flow from state to central servers.
Monthly factsheets are created at the state and national levels to provide a comprehensive picture of the progress made by all functional domains. The factsheet compares the progress made across States since the scheme’s commencement to the progress made each month. Some of the main data covered in the factsheet are the average claim size, the total number of pre-auths generated, pending approvals, and the nomenclature of the packages utilized at public and private facilities. The dashboards and factsheet identify triggers and outliers (if any), which are then drilled down to the district level.
Evidence is generated through evaluation studies in association with renowned research universities and partnerships with development agencies such as GIZ, WHO, and the World Bank in order to measure and comprehend the impact of PM-JAY. The goal of these evaluation studies is to determine the scheme’s impact on a variety of variables, including but not limited to out-of-pocket spending, access to health, health-seeking behavior, and so on. These studies provide crucial information for making evidence-based decisions and making mid-course modifications.
Fraud Prevention, Detection, and Control
It is vital to put in place a solid anti-fraud mechanism for a program of this scope, magnitude, and complexity as PM-JAY, not only from a financial standpoint but also to protect people’s health from unethical behavior and malpractices. The National Health Authority is aware of the problem and has taken many efforts since the program’s start to protect it. The following are some of the most important steps performed in this regard.
A.Policy and Design Level
For the selection of insurance companies, the Implementing Support Agency, and other service providers, a transparent tendering process was used. Penalty clauses and punitive action have been developed to deal with fraudulent activities on the part of any agency involved in delivering services under PM-JAY. Tightly worded legal documents for service delivery as per pre-defined Service Level Agreements have been developed with penalty clauses and punitive action to deal with fraudulent activities on the part of any agency involved in delivering services under PM-JAY.
The hospital empanelment procedure is based on a two-tiered system that includes district and state-level committees with representation from top authorities such as the civil surgeon, chief medical officer, and district nodal officers. The entire process is web-based, allowing hospitals to trace their empanelment status from application through approval by the State Nodal Age.
For all processes – beneficiary identification, transaction management system, funds flow, claims payment, and so on – IT systems and procedures have been established with checks and balances, defined roles and responsibilities, role-based logins, and audit trails. Furthermore, for speed and complete transparency, all pre-authorization and claims transactions are completed online.
The pre-authorization process has been developed to provide maximum efficiency while eliminating fraud and abuse. There are minimum requirements for claims investigation and medical audit. The introduction of all-inclusive package rates addressed the tendency of health care providers to overcharge, bill extra, and other related difficulties. However, enough leeway has been provided to treat individuals who require medical attention, and the list of treatments will be expanded as more experience and knowledge are gathered.
On August 27, 2018, the Minister of Health and Family Welfare issued Comprehensive Anti-Fraud Guidelines, outlining specific anti-fraud policies, processes, systems, and manpower at both the national and state levels.
National Health Agency Tollfree – 14555 has been established 24 hours a day, 7 days a week to facilitate beneficiary reporting and feedback Whistleblower Policy has been adopted at the NHA level and shared with States for comparable adoption.
B. Operational and System Level
- For SHAs, ISAs, and insurance partners, a capacity-building workshop for fraud control and medical audit was held. A fraud investigation manual was released to ensure a uniform and effective methodology and data collecting.
- Regular MIS and dashboards are used to monitor and analyze utilization trends, as well as to keep an eye on abuse-prone packages, dubious transactions, and hospitals.
- Top analytics businesses have been chosen to do a “proof of concept” for triggering suspicious transactions and entities using rule engines and an artificial intelligence layer on top of the Transaction Management System.
- The Kaizala app is being adapted for field investigations and medical audits, and testing is now underway.
Controlling abuse and leakages requires procedure-specific documentation and checklists, as well as IT integration. - Guidelines for adjudication and a capacity-building programme for SHAs and ISAs will be implemented.
- Keep an eye out for phoney websites, mobile apps that provide false information, and websites that collect money or personal information from the public.
National Anti Fraud Unit
Under PMJAY, NHA takes a “Zero Tolerance” policy against fraud and abuse. The National Anti Fraud Unit (NAFU) has been established with the primary responsibility for fraud and abuse prevention, detection, and deterrence under PM-JAY.
NAFU collaborates closely with State Anti-Fraud Units (SAFU) to ensure that the Scheme is implemented effectively and without any fraudulent or abusive conduct by any institution involved in PM-JAY implementation, including providers, and beneficiaries, ISAs, and payers.
NAFU carries out the following key activities:
- Provide leadership stewardship to the national anti-fraud efforts under PMJAY;
- Develop, review and update the national anti-fraud framework and guidelines based on emerging trends;
- Provide mentoring support to states in setting up and institutionalizing their in-state anti-fraud efforts;
- Capacity building of states on anti-fraud measures under PMJAY;
- Liaise with the national IT team/agency to ensure that the IT platform is periodically updated with fraud triggers based on the review of trends;
- Conduct audits and investigations of suspect cases/entities;
- Set up Forensics practice for the detection and triangulating of fraud/abuse related data with the overall service utilization trends emerging under PMJAY;
- Provide evidence-based insights to states on trends emerging from state-specific fraud data analytics;
- Handle all fraud-related complaints that the NHA may receive directly and liaise with the states from any complaints specific to states as per Anti-Fraud Guidelines
- Establish whistleblower mechanisms, public disclosure guidelines, and other deterrent measures.
Grievance Redressal
The grievance redressal system is designed to handle the issues of all PM-JAY stakeholders using natural justice principles while assuring cashless access to timely and high-quality care. For this objective, a three-tier Grievance Redressal Committee system has been established at the national, state, and district levels. The National Grievance Redressal Committee will be chaired by the CEO of NHA, while the State Grievance Redressal Committee will be chaired by the CEO of SHA. The Chairperson of the District Grievance Redressal Committee shall be the District Magistrate or an official of the level of Additional District Magistrate.
These committees will maintain and monitor the status of grievances, get additional information from parties involved, conduct hearings, review records, adjudicate and issue orders on grievances, and ensure that committee orders are followed.
Those who have been wronged can file complaints either by letter or through the NHA’s web portal (https://cgrms.pmjay.gov.in). For registering a grievance, other communication channels such as phone calls, faxes, e-mails, and SMS are also accepted. Grievances received through the National Call Centre (14555 / 1800 111 565) are also addressed through the Grievance Portal. The committee can also file complaints based on findings/reports from social media or public forums. Grievances will be handled either by the individual or organization responsible for taking action or by committees at the appropriate level, based on stated criteria.
However, the issue should be resolved within 30 days of receipt at any level. Any party’s right to appeal lasts for 30 days from the date of the decision. Failure to comply with the committee’s decisions within another 30 days will result in a penalty for the defaulter. The website allows users to assign and trace grievances to appropriate authorities, as well as check alert system compliance.
Call Centre
One of the most important aspects of one of the world’s largest government-supported health schemes of the size and complexity of PM-JAY is ensuring that eligible beneficiaries of the program can reach out to learn about the scheme’s details, have recourse to raise a query or a grievance, and seek information and support at any time of day or night, especially during the hour of need. If a significant portion of the beneficiaries is rural-based, even less educated, and less knowledgeable, the process must be further simplified and made simply accessible with the least amount of work and expense.
As a result, on August 24, 2018, the National Health Agency established a National Helpline – 14555 – that has been operational 24 hours a day, seven days a week since its start and has answered more than 42 lakh calls. The call center employs over 300 skilled agents who work around the clock to manage the calls, with plans to expand capacity in the future. The call center staff speaks all major regional languages.
The Helpline is toll-free, which means that the caller is not charged for making the call; NHA pays for it. The call center, which is open 24 hours a day, seven days a week, provides information and services to beneficiaries such as specifics about the scheme – coverage, benefits, how and where to use benefits, names and addresses of impaneled hospitals, and so on. Other stakeholders, including hospitals, Arogya Mitras, and field functionaries, also call the Helpline for assistance.
The call center also engages in outbound calling, with over 3 lakh outbound calls made to beneficiaries to collect feedback after releasing from the hospital, to learn about their experience, and to see if there were any challenges encountered during the procedure, among other things. Outbound calls are also made to hospitals to assist them in completing assistance, hand-holding, and training applications for providing services to PM-JAY beneficiaries, as well as to encourage them to increase pre-authorization.
Convergence
National Health Authority (NHA) and Employees State Insurance Corporation (ESIC) convergence (ESIC). The Employees State Insurance Corporation and the National Health Authority (NHA) have formed a collaboration (ESIC). This collaboration between Ayushman Bharat – Pradhan Mantri Jan Arogya Yojana (AB PM-JAY) and the Employees State Insurance Scheme (ESIS) would create an ecosystem in which ESIC beneficiaries can receive healthcare at ABPM-JAY impaneled hospitals and vice versa.
The coming together of PM-JAY and ESIC is a watershed moment in the country’s healthcare growth. This will take advantage of PM-established JAY’s network of high-quality service providers, as well as fixed health-benefit packages, to standardize services across schemes. Furthermore, it will increase the demand for health services in ESIC-approved facilities, which may be underutilized at the moment. This would help to upgrade the infrastructure and facilities of these facilities by utilizing funds paid under the PMJAY program.
In the first phase, ESIC beneficiaries in Ahmednagar, Maharashtra, and Bidar, Karnataka will be able to receive PM-JAY services in PM-JAY impaneled hospitals. The scheme’s beneficiaries will be eligible for all 1,393 secondary and tertiary packages, and the effort will be expanded to 102 districts with the goal of eventually covering the entire country.
Key Benefits of AB PM-JAY and ESIS convergence:
- ESIC beneficiaries will get access to healthcare providers under AB PM-JAY
- AB PM-JAY beneficiaries will be able to avail services in ESIC impaneled hospitals.
- Beneficiaries of ESIC can use their ESIS card to access free treatment at AB PM-JAY impaneled hospitals.
- Similarly, beneficiaries of AB PM-JAY can use their PM-JAY card to access free treatment at ESIC impaneled hospitals.
- For more information, beneficiaries can call ESIC tollfree number: 1800 112 526/ 1800 113 839
- Click here for the list of impaneled hospitals under AB PM-JAY.