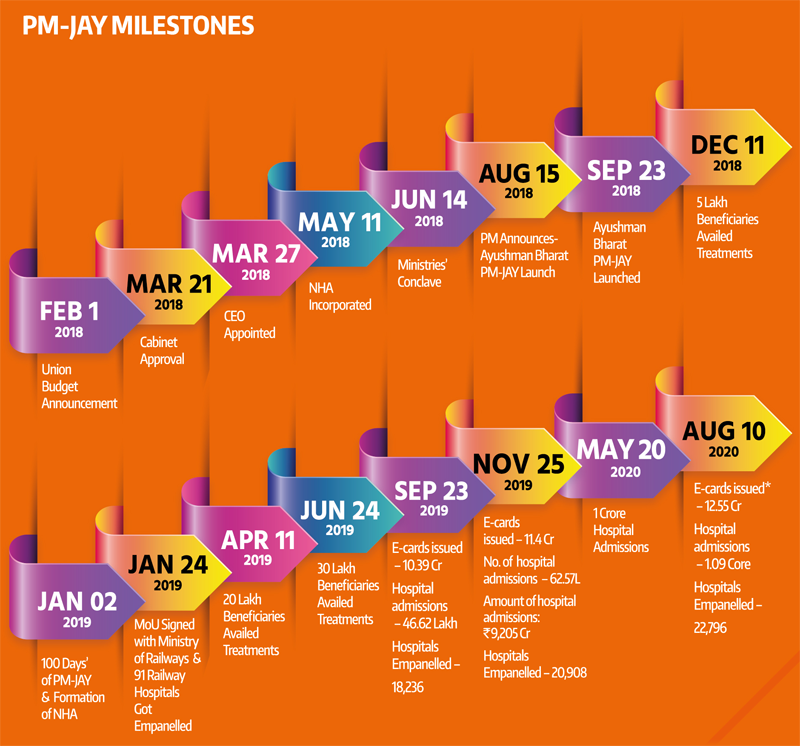
PM-JAY: Ayushman Bharat, the government of India’s flagship scheme, was created in response to the National Health Policy 2017’s recommendation to accomplish the vision of Universal Health Coverage (UHC). The goal of this project is to meet the Sustainable Development Goals (SDGs) and the underpinning pledge to “leave no one behind.”
Ayushman Bharat is an initiative to move away from a sectoral and segmented model to healthcare delivery and toward a comprehensive, need-based approach. This program aims to implement ground-breaking initiatives at the primary, secondary, and tertiary levels to address the healthcare system holistically (including prevention, promotion, and ambulatory care). Ayushman Bharat adopts a continuum of care approach, comprising of two inter-related components, which are –
- Health and Wellness Centres (HWCs)
- Pradhan Mantri Jan Arogya Yojana (PM-JAY)
1. Health and Wellness Centers (HWCs)
The Indian government announced in February 2018 that it would turn existing sub-centers and Primary Health Centres into 1,50,000 Health and Wellness Centres (HWCs). These clinics will provide Comprehensive Primary Health Care (CPHC), which will bring healthcare closer to people’s homes. They include free vital medications and diagnostic services, as well as maternal and child health care and non-communicable diseases.
Health and Wellness Centers are expected to provide a broader range of services to meet the primary health-care needs of the entire population in their service area, hence increasing access, universality, and equity in the community. The focus on health promotion and prevention is intended to keep people healthy by engaging and enabling individuals and communities to select healthy habits and make changes that minimize the risk of chronic disease and morbidity.
2. Pradhan Mantri Jan Arogya Yojana (PM-JAY)
Ayushman Bharat is a government-run healthcare program in India. PM-JAY is the world’s largest health assurance scheme, aiming to provide a health cover of Rs. 5 lakhs per family per year for secondary and tertiary care hospitalization to over 10.74 crores of poor and vulnerable families (about 50 crore beneficiaries) who make up India’s bottom 40%. The households included are based on the Socio-Economic Caste Census 2011 (SECC 2011) deprivation and occupational criteria for rural and urban areas, respectively. Before being renamed, PM-JAY was known as the National Health Protection Scheme (NHPS).
The Rashtriya Swasthya Bima Yojana (RSBY), which had been launched in 2008, was absorbed into it. As a result, the coverage mentioned under PM-JAY includes families who were insured under RSBY but are not in the SECC 2011 database. The government entirely funds PM-JAY, and the expense of implementation is split between the federal and state governments.
Key Features of PM-JAY
- PM-JAY is the world’s largest government-funded health insurance/assurance scheme.
- It covers secondary and tertiary care hospitalization in India’s public and private impaneled hospitals up to a maximum of Rs. 5 lakhs per family per year.
- These benefits are available to around 10.74 crore poor and disadvantaged families (roughly 50 million people).
- PM-JAY enables beneficiaries to pay for health care services at the point of service, which is the hospital.
- PM-JAY aspires to assist in mitigating catastrophic medical costs, which force over 6 crore Indians into poverty each year.
- It pays for up to three days of pre-hospitalization and up to fifteen days of post-hospitalization expenses, such as tests and medications.
- There are no restrictions on the size, age, or gender of the family.
- From day one, all pre-existing conditions are covered.
- The scheme’s benefits are portable across the country, which means that beneficiaries can seek cashless care at any impaneled public or private hospital in India.
- Around 1,393 procedures are included in the services, which cover all expenditures associated with treatment, including but not limited to pharmaceuticals, supplies, diagnostic services, physician’s fees, hotel charges, surgeon charges, OT and ICU charges, and so on.
- Public hospitals are reimbursed on a level with private hospitals for healthcare services.
Benefit Cover Under PM-JAY
Benefits coverage under various government-funded health insurance programs in India has traditionally been capped at INR 30,000 to INR 3,00,000 per family per year, resulting in a fragmented system. PM-JAY provides cashless coverage of up to INR 5,00,000 per year for specified secondary and tertiary care conditions to each qualified family. The policy covers all expenses associated with the following components of the therapy.
- Medical examination, treatment, and consultation
- Pre-hospitalization
- Medicine and medical consumables
- Non-intensive and intensive care services
- Diagnostic and laboratory investigations
- Medical implantation services (where necessary)
- Accommodation benefits
- Food services
- Complications arising during treatment
- Post-hospitalization follow-up care for up to 15 days
The benefits of INR 5,00,000 are available on a family floater basis, which means they can be utilized by one or all family members. The RSBY had a five-member family cap. However, in light of the lessons learned from such programs, PM-JAY has been constructed in such a way that there is no restriction on the size of families or the age of individuals. Additionally, pre-existing disorders are covered from day one. This means that any eligible person who was previously covered by PM-JAY will now be able to receive treatment for all of their medical issues under this program beginning on the day they enroll.
Why PM-JAY: A Background
Over the last few decades, the world’s attention has been focused on India, as its economy has consistently ranked among the world’s top three fastest-growing economies. Despite great progress in various sectors, India is still classed as a Lower Middle-Income Country (LMIC) by the World Bank, mostly due to inconsistent socioeconomic and health statistics.
According to statistics, more than 20% of India’s population still lives on less than $1.9 per day (2011 PPP). According to a World Bank prediction, more than 34% of India’s population will be between the ages of 15 and 35 by 2021. India can be quite hopeful about sustained economic growth for a few more decades until a greater reliance ratio creeps in.
However, the apparent benefits of a larger demographic dividend are jeopardized by India’s epidemiological change, which has created an unprecedented “triple burden of sickness.” While the quest to eradicate major communicable diseases continues, the population continues to endure a disproportionate burden of non-communicable diseases (NCDs) and injuries. This results in a sustained increase in the demand for health care.
However, with a total population of over 1.3 billion, India’s provision of adequate and cheap healthcare falls short. The data demonstrate an overwhelming preference for private health care services, which account for approximately 70% of all visits for health care requirements in India and account for 50% of total hospital beds. However, the majority of private-sector providers are extremely modest on an individual basis (with less than 25 beds). Additionally, they are unregulated, have variable levels of care, and are concentrated in large metropolises or urban neighborhoods, leaving a significant gap in health services for India’s disadvantaged people.
However, as the world’s second most populated country, India’s public hospitals are inevitably overworked. Their utilization varies considerably, and they frequently face difficult constraints due to a lack of appropriate money, a paucity of educated health personnel, and an unpredictable and frequently deficient supply of pharmaceuticals and equipment, all of which impair their operation.
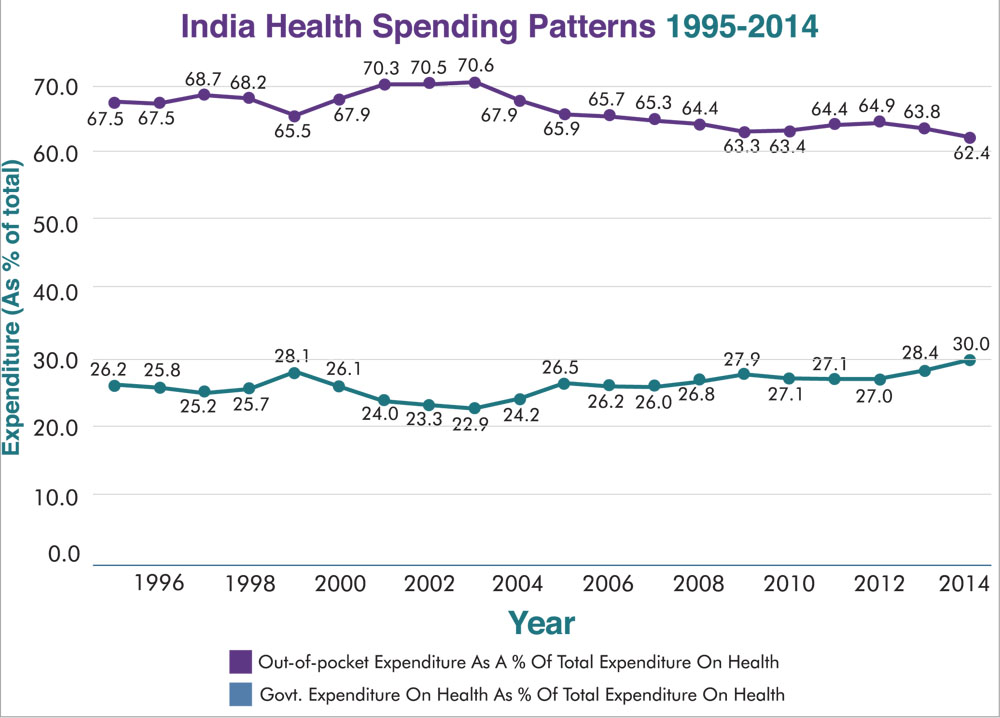
One of the primary causes of this condition is the country’s public health care system’s continual underfunding. Over the previous two decades, India’s overall health expenditure has been stable at around 1.2 percent of GDP (Source: National Health Accounts, 2015). India spends only 21% of its overall health expenditure on government revenue and up to 62% on out-of-pocket expenses (Source: National Health Accounts, 2015). As a result, it has been determined that rising health care costs, combined with high out-of-pocket expenses, are a significant source of poverty in India.
Not only does it keep people impoverished, but it also reintroduces nearly 6 crore Indians to poverty each year. The following graph illustrates this scenario succinctly by comparing the OOP to overall health expenditure over a two-decade period.
Historically, the Central and various State Governments have attempted to enhance demand-side financing by introducing a variety of government-funded health insurance plans. The Rashtriya Swasthya Bima Yojana (RSBY) was launched at the government level with an annual benefit of INR 30,000 per family and covered primarily secondary care hospitalization, but many State programs covered tertiary care diseases. However, these plans operated independently of the country’s wider health care system, significantly fragmenting risk pools. Additionally, none of these programs were connected to basic health care.
To address these issues, the Indian government took a two-pronged approach through Ayushman Bharat. The strategy’s first component was illness prevention and health promotion, with the goal of containing the growing epidemic of non-communicable diseases. This was to be accomplished by converting the existing network of Sub-Centers and Primary Health Centers into Health and Wellness Centers (HWC). Over the following few years, about 150,000 HWCs will be established throughout the country, with the goal of reducing the overall illness burden and hospitalization needs of the population.
The second component was the launch of the Pradhan Mantri-Jan Arogya Yojana (PM-JAY), which aims to establish a system of demand-driven health care reforms that meet the immediate hospitalization needs of eligible beneficiary families in a cashless manner, thereby shielding the family from catastrophic financial shock. In the long run, the PM-JAY hopes to enhance the availability of its services through its incentive system. The private sector is projected to expand in unserved parts of Tier-2 and Tier-3 cities as demand increases.
PM-JAY will create an incentive for public hospitals to prioritize disadvantaged patients and will provide a mechanism for them to collect additional income to upgrade their infrastructure and cover service deficiencies. PM-JAY has absorbed the previous RSBY and also works in conjunction with a variety of state-funded health insurance/assurance programs.
Due to its size, PM-JAY is the world’s largest health insurance/assurance scheme, providing health coverage to over 10.74 crore poor families, or a staggering 50 crore Indians who account for 40% of the country’s poor. It is entirely government-funded and covers a wide array of secondary and tertiary care hospitalizations. PM-primary JAY’s purpose is to reduce catastrophic out-of-pocket health expenditures for its poor population by increasing access to high-quality health care. Further details about its evolution, planning, eligibility, and state-by-state implementation will be explored in the sections that follow.
Coverage under PM-JAY
Including the poorest and most vulnerable members of any country’s population into its health insurance program is frequently the most difficult task, as they cannot pay any premium and are the most difficult to reach. Often, they are also illiterate, necessitating a very different strategy for raising awareness. This is true for the majority of Lower and Middle-Income Countries (LMICs), including India.
As a result, PM-JAY has been extended to the bottom 40% of a poor and vulnerable population. This equates to approximately 10.74 crores (100.74 million) households in absolute terms. Households are included based on deprivation and occupational criteria from the 2011 Socio-Economic Caste Census (SECC 2011), respectively, for rural and urban areas. Additionally, this number includes households that were covered by the RSBY but not included in the SECC 2011 database.
The SECC entails classifying families according to their socioeconomic condition. It applies exclusion and inclusion rules and determines which homes are automatically included and excluded. Rural households that are included (but not excluded) are then ranked according to their level of deprivation under seven deprivation criteria (D1 to D7). Urban households are classified according to their occupations.
In keeping with the Government’s strategy of utilizing the SECC database for social welfare programs, PM-JAY also uses this data to identify targeted recipient households.
Rural BeneficiariesPM-JAY encompassed all such families that met at least one of the following six deprivation criteria (D1 through D5 and D7) and were automatically included (destitute/living on alms, manual scavenger households, primitive tribal group, legally released bonded labor):
- D1- Only one room with kucha walls and kucha roof
- D2- No adult member between ages 16 to 59
- D3- Households with no adult male member between ages 16 to 59
- D4- Disabled member and no able-bodied adult member
- D5- SC/ST households
- D7- Landless households deriving a major part of their income from manual casual labor
Urban BeneficiariesFor urban areas, the following 11 occupational categories of workers are eligible for the scheme:
- Ragpicker
- Beggar
- Domestic worker
- Street vendor/ Cobbler/hawker / other service provider working on streets
- Construction worker/ Plumber/ Mason/ Labour/ Painter/ Welder/ Security guard/ Coolie and other head-load worker
- Sweeper/ Sanitation worker/ Mali
- Home-based worker/ Artisan/ Handicrafts worker/ Tailor
- Transport worker/ Driver/ Conductor/ Helper to drivers and conductors/ Cart puller/ Rickshaw puller
- Shop worker/ Assistant/ Peon in small establishment/ Helper/Delivery assistant / Attendant/ Waiter
- Electrician/ Mechanic/ Assembler/ Repair worker
- Washer-man/ Chowkidar
While PM-JAY employs the SECC to determine household eligibility, many States have previously implemented their own health insurance programs with pre-identified beneficiaries. Thus, states have the option of using their own PM-JAY database. They will, however, need to ensure that all eligible families as identified in the SECC database are likewise covered.
Expansion of coverage by States under PM-JAY and convergence
Over the last couple of decades, different states have implemented their own health insurance/assurance programs. The majority of these plans cover only tertiary care issues. The benefits provided by these programs are primarily available inside the limits of the states, with the exception of a few smaller states that have impaneled a few hospitals outside their borders. Only a few States had merged their schemes with the defunct RSBY program, and the majority of them continued to operate separately. This was owing to the RSBY’s lack of flexibility in design, which originally aided in rapid scale-up but became a challenge over time and provided the States with limited flexibility.
Even though these programs targeted the poor and disadvantaged, eligibility requirements and databases varied significantly between states. Few states made use of the food subsidy database, while others established their own for their welfare programs.
PM-JAY’s objectives were to assure comprehensive coverage for catastrophic illnesses, reduce catastrophic out-of-pocket expenses, increase access to inpatient treatment, reduce unmet needs, and consolidate diverse health insurance systems across the States. Additionally, PM-JAY would set national standards for a health assurance system and will facilitate care portability across borders.
At the implementation level, states have the option of using their own database if they are currently operating a health insurance/assurance program and we are covering more families than those eligible under the SECC 2011 database. The such States, however, shall guarantee that all families eligible for benefits under the SECC are covered and not denied benefits.